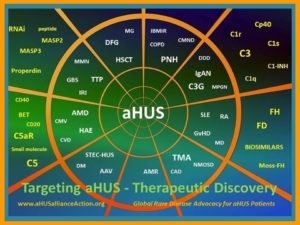
The aHUS Alliance presents an overview of a small segment of orphan drug research and development, with the potential for advancements in 2017 that may bring new therapeutic drugs to treat patients with atypical HUS. Research in the field of complement-mediated diseases in 2016 became a faster flowing river of information that sought new levels and touched upon new shores. International research collaboration and translational science appears to increasingly cut across disciplines and medical specialties, providing a continually evolving landscape with expanded potential for advancement in 2017 regarding new therapeutic drugs in development which might hold promise as future treatment options for aHUS patients.
As with most exceptionally rare diseases, atypical hemolytic uremic syndrome (aHUS) is not well known1 by clinicians, although that is beginning to change with the aHUS pediatric global consensus2 in 2015 and conclusions from the 2016 KDIGO global Controversies Conference regarding improved outcomes for patients with aHUS and C3 glomerulopathy3. An additional barrier for those seeking information about aHUS is the variance in spelling4 which is further compounded by the various ways this disease is categorized or grouped in the literature, such inclusion of aHUS research as under the generalized terms “complement mediated diseases” and “thrombotic microangiopathies” (TMA). Those seeking clinical trials open to aHUS patients suffer similar difficulty uncovering information, since 22 studies can be found on www.ClinicalTrials.gov5 utilizing the search term “atypical HUS” with 55 entries found by changing the search term to “aHUS”.
Global investigation and development of innovative therapeutic drugs is a complex process, especially in light of additional challenges for orphan drugs and biopharmaceuticals. Presented here are links to various therapeutic agents in development, as well as research topics and additional disease information which may impact knowledge, provide insights, or affect future developments related to aHUS. Increased knowledge of immune and Inflammatory mechanisms may aide better understanding of aHUS, to include diseases which share a trait in common with the three main clinical characteristics of aHUS: microangiopathic hemolytic anemia (to include red blood cell destruction), acute kidney injury (AKI), and thrombocytopenia (platelet deficiency).6 Eculizumab was approved for therapeutic use with aHUS patients in 20117 but initially was investigated as a complement inhibitor for PNH patients, so it’s logical to keep aware of new information related to that rare disease and additionally also monitor therapeutic drug development and research findings for certain other diseases.
Investigations into novel drug developments for complement-mediated diseases have approached new therapeutic options on all three pathways, targeting different stages and binding sites. The complement system is a critical part of the immune system, with three biochemical arms: classical, lectin (MBL), and alternative pathways. Multiple approaches exist to build a “complement arsenal” 8. With new complement inhibitors under investigation, some target early in the complement cascade (upstream) and others with later intervention points (downstream). Activation of complement pathways and its dysregulation, a hallmark of aHUS activity, plays a central role in many diseases. Research tends toward a growing number of disease associations, along with improved insight into immune cross-talk mechanisms. Since medical and research professionals are much better qualified to present a full review of the literature and to detail specifics of therapeutics under development that may hold promise for aHUS patients, recognize that information here serves merely as a starting point to delve deeper.
Therapeutic Drug Discovery
aHUS and other Complement Mediated Diseases
Check for updated information on Clinical Trials at www.ClinicalTrials.gov
Learn about Clinical Trials & Stages of Development: http://www.nlm.nih.gov/services/ctphases.html
See Appendix: Table of Diseases: Potential for Cross-Over to aHUS Research
Advancements in disease knowledge and treatments could be accelerated by collaboration and data sharing, but genomic and clinical data largely remains collected, studied, and held in silos that often isolate information by disease, institution, and/or nation.9 Progress in rare disease research and investigational drug development is understandably hampered due to a core concept of rare diseases, the very small patient populations. Valid issues and barriers exist in the highly competitive field of research as well as throughout the pharmaceutical and biotechnology industries, particularly regarding proprietary information and intellectual property concerns. Privacy rights and informed consent present legal and access challenges on an international stage, and become key considerations for responsible data sharing and collaborative efforts among researchers, nations, rare disease registries, and genomic projects. For those reasons, it is particularly impressive to see effective trans-disciplinary research efforts that involve multi-national, holistic collaborations in rare disease research, at conferences, and for global registries.
As the future of aHUS therapeutic drugs continues to unfold throughout 2017, so will advancements in biotechnology realms. Increasing rates of kidney failure have boosted the need for new and better options, to include expanded exploration of artificial kidneys and biotechnology such as ‘kidneys on a chip’. Genomics, gene editing, and CRISPR technology are hot topics with multiple applications in the rare disease arena, both for research organizations and drug discovery companies. While generic drugs simply copy a chemical compound, creating biosimilar drugs of existing biopharmaceuticals is much more difficult. Since biosimilars and biologics are made from living materials, replication presents special challenges although successful biosimilars may mean lower treatment costs for patients and therefore potential for broader adoption and access. In the 2016 aHUS Global Poll 67% of respondents noted that their specialist or medical team had discussed aHUS treatment cost with the patient and their family, with access to treatment highlighted as a key concern for patients, families, and advocacy groups.
Conferences in the medical, rare disease, and biotech arenas provide a rich source of information in addition to gaining knowledge via a review of the literature. Hints of possible aHUS advancements can be referenced in such diverse areas as inflammatory and immunology research, with new information presented across disciplines at nephrology, hematology, genetic, renal, complement, and other conferences. Given all the information, all the research, all the clinical expertise, we still jointly (and rightly) focus on the same basic goal of improving patient outcomes. At the heart of all areas and all efforts in both research and clinical settings, from bench to bedside, is the patient.
Patient-centered care includes establishing a respectful relationship where patients feel involved, informed, and involved in their care. Much has been written about patient engagement and its value, and patient organizations can help facilitate patient involvement at all stages and with all aspects of research, drug development, and clinical trials. The aHUS Alliance Directory lists known aHUS patient groups and organizations, providing networking assistance to allow those with an interest in aHUS to establish direct connection with various nations and groups around the world. The 2016 aHUS Global Poll, with 233 respondents in 23 nations, provided both data and insight into the aHUS patient experience, amplifying their voice relative to interests, needs, and views on all aspects of treatment and care. Patients and pediatric caregivers offered opinions on a wide range of important topics to include various research areas, drug development, and access to treatment. The aHUS Alliance is sponsoring an “Patients’ Voice: aHUS Research Questions”, to launch on Rare Disease Day 28 February 2017, echoing the 2017 Rare Disease Day theme of “Research” by engaging the aHUS community around the world to state questions about aHUS research.
Connecting scientific and technology advancements to aHUS research helps patients, caregivers, and families learn about their diagnosis and provides background for deeper understanding of discussion they may have with their specialists and care team. Collaboration and connectivity among stakeholders’ efforts was central to the first aHUS patients’ research agenda, resulting in the Orphanet article “An innovative and collaborative partnership between patients with rare disease and industry-supported registries: the Global aHUS Registry” in which the aHUS Alliance revealed a list of priority aHUS research topics within the context of the global registry for aHUS patients. From registries to research, from conferences to clinical trials, consider adding the patient perspective – everything for patients, with patients. Who better than patients to voice opinion about the new therapeutic options, note concerns about drug cost and access, or comment on research directions and priorities? In commerce, one would not bring a product to market without focus groups and a vast understanding of the needs and concerns of the end-user of that product. In 2017, may the coming year be rich with new knowledge, innovative research, broad collaborations and yes – hope for major advancements in therapeutic drugs.
January 2017
L Burke
About the aHUS Alliance
As an international group of aHUS patient organizations, the aHUS Alliance reaches out to provide news and insights into key topics of high interest to the aHUS community through website, Facebook, and Twitter content. Specific groups and nations involved in aHUS advocacy around the world can be viewed in the aHUS Directory, a list of known patient associations or outlets with an aHUS website or social media presence.
Contact the aHUS Alliance by email at: info@ahusallianceaction.org
Citations
1
aHUS Alliance Fact Sheets. aHUS Key Facts & Information (Sept 2016): http://ow.ly/dttf304bJGZ
aHUS Facts – a Brief Look (Sept 2016): http://ow.ly/UetJ304bKcS
2
Loirat, C, Fakhouri, F, Ariceta,G et al. An international consensus approach to the management of atypical hemolytic uremic syndrome in children. Pediatr Nephrol (2016) 31: 15. doi:10.1007/s00467-015-3076-8.
3
Goodship TH, Cook HT, Fakhouri F, Fervenza FC, Frémeaux-Bacchi V, Kavanagh D, Nester CM, Noris M, Pickering MC, Rodríguez de Córdoba S, Roumenina LT, Sethi S, Smith RJ; Conference Participants. Atypical hemolytic uremic syndrome and C3 glomerulopathy: conclusions from a “Kidney Disease: Improving Global Outcomes” (KDIGO) Controversies Conference. Kidney Int. 2016 Dec 15. pii: S0085-2538(16)30604-4. doi: 10.1016/j.kint.2016.10.005 (Disclosure: Author of this article L Burke is listed as a conference participant.)
4
Woodward, L. A Rose by Any Other Name – What’s the Fuss? 26 Oct 2016 article.
5
aHUS Clinical Trials: Search term “aHUS”. Multiple spellings and forms are exist as search terms, to include “atypical HUS” and “atypical hemolytic uremic syndrome”.
6
Kavanagh D, Goodship TH, Richards, A. Atypical Hemolytic Uremic Syndrome. Semin Nephrol 2013 Nov; 33(6): 508–530. doi: 10.1016/j.semnephrol.2013.08.003
7
FDA Press Release- The U.S. Food and Drug Administration. FDA approves Soliris for rare pediatric blood disorder. 23 Sept 2011.
8
Ricklin D and Lambris, J. Complement in Immune and Inflammatory Disorders: Therapeutic Interventions. The Journal of Immunology April 15, 2013vol. 190 no. 8 3839-3847. doi: 10.4049/jimmunol.1203200
9
Goodhand, Peter et al. (The Global Alliance for Genomics and Health) A federated ecosystem for sharing genomic, clinical data. Science 10 Jun 2016: Vol. 352, Issue 6291, pp. 1278-1280
DOI: 10.1126/science.aaf6162
Additional Resources
Complement & Therapeutic Options
Antwi-Baffour S et al. The relative merits of therapies being developed to tackle inappropriate (‘self’-directed) complement activation. Auto Immun Highlights. 2016 Dec; 7(1): 6.
Joost PM et al. Complement in therapy and disease: Regulating the complement system with antibody-based therapeutics. Molecular Immunology. Volume 67, Issue 2, Part A, October 2015, Pages 117–130
Morgan, B. Paul and Harris, Claire L. Complement, a target for therapy in inflammatory and degenerative diseases. Nature Reviews: Drug Discovery. Nature Reviews Drug Discovery: 14, 857–877 (2015) doi:10.1038/nrd4657. Published online: 23 October 2015.
Reis E et al. Applying complement therapeutics to rare diseases. Clin Immunol. 2015 Dec; 161(2): 225–240. doi: 10.1016/j.clim.2015.08.009
Ricklin D and Lambris J. Complement in Immune and Inflammatory Disorders: Therapeutic Interventions. doi: 10.4049/jimmunol.1203200The Journal of Immunology April 15, 2013vol. 190 no. 8 3839-3847
Thurman JM and Nester CM. All Things Complement. CJASN June 2016CJN.01710216 doi: 10.2215/CJN.01710216
Wong E, Goodship THJ, Kavanagh D. Complement therapy in atypical haemolytic uraemic syndrome (aHUS). Mol Immunol 2013 Dec 15; 56(3): 199–212.
Note: Other aHUS Research topics – see the aHUS Alliance List of aHUS Research
aHUS Alliance – Assets
aHUS Publications – List of aHUS Research
aHUS White Papers – Access to aHUS Treatment and aHUS and Dialysis Insights
2016 aHUS Global Poll
Orphanet – Joint Collaboration between Patients and the aHUS Global Registry
Directory of aHUS Patient Organizations and Advocacy
Info Centre
Diseases/Disorders: Potential for Cross-Over to aHUS Research
| AAV | (ANCA)-associated vasculitis Note: ANCA – anti-neutrophil cytoplasmic Abs |
| AMD | Age-related Macular Degeneration |
| AMR | Antibody mediated rejection |
| CAD | Cold Agglutinin Disease |
| CAD | Coronary Artery Disease |
| CMV | Cytomegalovirus |
| C3G | C3 glomerulopathy, Subtypes: Dense deposit disease (DDD) and C3 glomerulonephritis (C3GN) |
| CMND | Complement-Mediated Neurodegeneration |
| COPD | Chronic Obstructive Pulmonary Disease |
| CVD | Cardiovascular Disease |
| DDD | Dense Deposit Disease (see also C3G) |
| DFG | Delayed Graft Function |
| DM | Dermatomyositis |
| GBS | Guillain Barr Syndrome |
| GvHD | Acute Graft v Host Disease |
| HAE | Hereditary Angioedema |
| HSCT | Hematopoietic Stem Cell Transplant |
| IBMIR | Instant Blood-mediated Inflammation Reaction |
| IgAN | Immunoglobulin A Nephropathy (form of glomerulonephritis) Note IgA – Immunoglobulin A |
| IRI | Ischemia-reperfusion Injury |
| MG | Myasthenia Gravis |
| MMN | Multifocal Motor Neuropathy |
| MPGN | Membranoproliferative glomerulonephritis |
| NMOSD | Relapsing Neuromyelitis Optica Spectrum Disorder |
| PNH | Paroxysmal Nocturnal Hemoglobinuria |
| RA | Rheumatoid arthritis |
| SLE | Systemic Lupus Erythematosus |
| STEC | HUS – Shiga toxin-releasing Escherichia coli-Hemolytic Uremic Syndrome |
| TMA | Thrombotic microangiopathy (often plural) |
| TTP | Thrombotic Thrombocytopenic Purpura |
Note: Research done for other complement-mediated diseases, or those with similar underlying mechanisms, may provide knowledge to advance aHUS research and therapeutic drug discovery. Listed are some diseases for which future investigations may provide cross-over information for aHUS researchers.
