
Atypical HUS patients who have progressed to kidney failure and do not have access to a complement inhibitor like Eculizumab have to be on dialysis for many years. (Read 1st Dialysis Diaries article here and the 2nd on the topic of diet & fluids here). Being on dialysis for a long time primarily impacts the heart. This is due to the fluid that accumulates in the body between two dialysis sessions.
The human heart has evolved over millennia to handle about five litres of blood. This blood is pumped continuously by the heart and it circulates in the entire body. For those with healthy kidneys, fluid that is ingested either in the form of water or as part of the food eaten is partly retained by the body and whatever is not needed is excreted in the form of urine. For those on dialysis, most of the fluid remains in the body until the next dialysis session.
For dialysis patients, therefore, there is almost always some excess fluid in the body. This is extra work for the heart which is used to pumping only about five litres but now has to pump all this excess fluid. Some patients who adhere to their fluid restrictions would have not more than a litre of extra fluid in them. Other patients can have as much as five litres extra in them. So, the heart has to pump from 20% to 100% extra than what it is designed for.
Removal of this fluid is another major problem in dialysis patients. While the excess fluid consumed is gradually eliminated by those with healthy kidneys, those on dialysis have to get rid of all the excess fluid in what is typically a four hour dialysis session. The human body can safely lose about 400 ml of fluid per hour. This varies from person to person with smaller built people able to lose a little less while large people can lose a little more without having any complications.
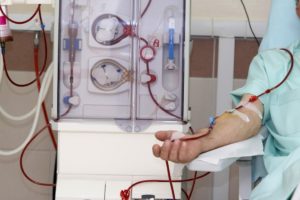
However, during dialysis, the fluid gained between two treatments has all to be removed in the four hour session. If someone has anything more than 1.6 litres of excess fluid, they would have to pull off fluid during their dialysis session at more than the recommended rate. This can cause a condition called “Myocardial stunning” which happens due to rapid removal of fluid from the body.
All this is hugely detrimental to the heart’s health in the long term. To begin with, it adjusts to the extra work. Over time, however, it starts growing in size due to the additional volume of fluid it handles on a regular basis. This can happen only up to a certain point. After a certain duration of time, it simply fails as it cannot handle any more fluid.
Most people on dialysis die of cardiac issues rather than any problem related to the kidney directly. The additional load on the heart is the primary cause of this. Dialysis patients have a thirty times higher risk of death from cardiovascular problems compared to the general population.(1)
There are a number of other issues that dialysis patients can face related to the heart. These are the more traditional conditions like arrhythmias, coronary artery disease, valvular heart disease etc. Dialysis patients are equally susceptible these conditions as the general population.
Studies show that Cardiac disease is the largest single cause of death for both hemodialysis and peritoneal dialysis patients, accounting for 43% of all-cause mortality (2). Factors peculiar to long term dialysis are implicated in death due to cardiac disease. Fluid overload, especially over the weekend, when most dialysis patients have their two-day gap between treatments (called the ‘killer weekend’) causes the heart to overwork and eventually fail.
There are some things that can be done to reduce the risk of death due to Cardiac Disease. Staying within the allowed limit of the daily fluid intake and reducing the amount of salt consumed are two obvious things dialysis patients can do. Apart from this, increasing the frequency of dialysis helps. Some patients do dialysis 5-6 times a week. This results in reduced accumulation of fluid in the body since the number of hours between two dialysis sessions is reduced. Another thing which some patients do is to do longer duration dialysis. Instead of doing the typical four hour sessions, they do seven or eight hours. This allows the fluid to be removed in a more gradual manner. This reduces the risk of Myocardial Stunning.
Dialysis patients must also maintain healthy habits related to diet and exercise since they are also at risk of general heart conditions like the rest of the population.
In summary, the heart plays a very important role in kidney disease. Read more about this relationship in the aHUS Alliance’s blog on Cardiorenal syndrome. Fluid overload is a major cause of cardiac issues in dialysis patients. There are ways by which the risk can be reduced. Adopting some or all these ways is very important in aHUS patients without access to a complement inhibitor because they need to be on dialysis for several years, potentially lifelong.
This article is the third in the aHUS Alliance series, Dialysis Diaries.
Author Kamal D Shah has been on dialysis for the last 22 years. He is founder of Atypical HUS India, and co-founder of NephroPlus Dialysis Centres, India’s largest Dialysis Centre Network. He is one of the directors of aHUS Alliance Global Action, whose most recent collaboration includes the KDIGO publication on Increasing Access to Integrated ESKD Care. Click HERE to read the aHUS Alliance interview with Kamal D Shah. Click HERE to read his blog.
References Cited
- Cardiorenal Syndrome: The Relationship of Heart and Kidney Health by Linda Burke, March 2019

