How rare is ‘aHUS Rare’?
If you or a loved one has been diagnosed with atypical HUS, it’s likely the medical team also stated “It’s a very rare disease”. But what does that actually mean?
Definitions of a Rare Disease Vary: But Why & How?
In the United States, the Orphan Drug Act (ODA) of 1983 defines a rare disease as one affecting fewer than 200,000 Americans — roughly fewer than 60 people per 100,000, or fewer than 600 per million. The purpose of the ODA (M Herder, PLoS Med. 2017) was to offer incentives which encouraged pharmaceutical companies to develop drugs for rare diseases—a sector often ignored because limited patient numbers typically result in a failure to recover R&D investments
In Europe, the European Medicines Agency (EMA) sets the threshold at fewer than 1 in 2,000 people — that’s fewer than 50 per 100,000, or under 500 per million. This definition shapes which medicines qualify as within the EMA framework as “orphan drugs” — a designation that encourages pharmaceutical companies to develop treatments for diseases that would otherwise be overlooked.
Atypical HUS doesn’t just meet the defined thresholds of rare disease — it falls dramatically below them. Estimates suggest that aHUS affects only about 2 to 9 people per million worldwide. That places atypical HUS firmly in a different category altogether, not only rare but as an exceptionally rare disease indeed.
Not Common, but an ‘Ultra-Rare’ Disease?
Ultra-rare diseases are generally defined as those affecting fewer than 1 in 50,000 people — fewer than 2 per 100,000, or under 20 per million. While the term doesn’t have an official legal definition, ultra-rare diseases are generally defined as those affecting fewer than 1 in 50,000 people — fewer than 2 per 100,000, or under 20 per million.
With only 2 to 9 cases per million people, atypical HUS is significantly lower than this ‘ultra-rare’ threshold of 20 per million.
The ‘ultra rare’ term doesn’t have an official legal definition but it is recognized in medical literature, appearing almost two thousand times and in more than 500 citations in PubMed, the research database maintained by the National Library of Medicine and the National Institutes of Health (Hughes et al., 2005).

So How Many People Actually Have aHUS?
That question is harder to answer than it might seem. The estimate of 2 to 9 aHUS patients per million people varies widely, and there are several reasons for that. First, countries differ in how they define and classify aHUS. Second, some nations track the disease more closely than others. Third — and importantly — researchers and clinicians suspect aHUS is significantly under-reported. Diagnosing aHUS is complicated by the absence of a single definitive test, forcing doctors to rule out other conditions before atypical HUS can be confirmed — a ‘diagnosis of exclusion’ process that leaves patients vulnerable to misdiagnosis or delays in appropriate treatment.
There is also a more technical reason aHUS patient counts differ: the distinction between incidence and prevalence — two related but different ways of counting disease.
Incidence refers to the number of new cases that are diagnosed or develop over a specific period of time — typically one year. Think of it as the rate at which people are newly joining the group of people diagnosed with this disease. Prevalence refers to the total number of existing aHUS cases — both newly diagnosed and those living with the disease from prior years — at any given point in time. Think of it as the total size of the aHUS patient population right now.

What is Atypical HUS?
It’s difficult for aHUS patients and their families to describe this rare disease to friends and coworkers, especially since sources usually offer descriptions heavy with medical terms . Think of it this way. Atypical hemolytic uremic syndrome (tagged as atypical HUS, aHUS, primary TMA or cmTMA) is an exceedingly rare and life-threatening disease. In aHUS, a part of the body’s own immune system misfires. Instead of protecting the body, it attacks the healthy cells that line blood vessels. The result: tiny, dangerous blood clots form inside those vessels. Those clots block the normal flow of blood to vital organs. The word ‘uremic’ in the disease’s full name atypical hemolytic uremic syndrome indicates that out of all organs, the kidneys take the hardest hit. People with aHUS experience varied degrees of kidney damage, though how serious that damage becomes, and potential harm to vital organs like the brain or heart, can differ greatly from one person to the next.
While the description above glosses over or omits key points for the sake of brevity, learn more by exploring the resources at the end of this article.
Expert Care for aHUS Patients?
Because atypical HUS is so very rare, most doctors never see a single case of aHUS throughout their career. Unlike more common medical conditions, there is no simple way to search for and find a dedicated ‘aHUS specialist’. Patient care is typically led by nephrologists, due to the kidney involvement (hence the word ‘uremic’ in atypical hemolytic uremic syndrome), or hematologists, because of the effects on blood clotting, red blood cells, and platelets. In your search for a physician near you, know that aHUS may be described under broader medical terms like ‘thrombotic microangiopathy (TMA)’ or ‘complement-mediated disease’, reflecting that in most cases aHUS results from a malfunction in the complement pathway that causes the immune system to cause damage throughout the body, rather than carrying out its protective role.
Despite the status of atypical HUS as an ultra-rare disease, patients can request assistance through their doctors, hospitals, and case managers. Additionally there are some established pathways for your local medical team to connect directly with world-class aHUS experts. Members of the aHUS Alliance Global Action team in 2012 began creating an international network acting as an informal ‘Doc to Doc Directory’, to establish a way for local medical teams to connect with world-class clinicians and aHUS researchers. Our website hosts a list of aHUS/TMA study centers, a resource which highlights institutions with deep clinical and research experience and potentially suggest avenues of assistance available near your region. We extend our deepest thanks to these clinicians and investigators worldwide who volunteer their time and talents to make such collaborative support networks possible.
Our appreciation goes out to all medical professionals and research teams who strive toward filling in the many knowledge gaps related to aHUS/TMA, and those who strive to solve issues surrounding challenges for the global aHUS community.
Website Assets – Basic Info for aHUS Families
Atypical HUS Fact Sheet 2025 -Sept – 2026 edition
aHUS Info Centre: Research (a ‘virtual library’), Key Resources Index, Assets in FR/ES/PT & MORE
More Articles about Patient Numbers
Numbers of aHUS patients (Nov 2024)
Are there 3000 aHUS patients in the USA? (July 2023)
Is incidence of aHUS really “2 per million”? (March 2023)
Again, just how many aHUS patients are there? (Aug 2020) Incidence & prevalence, patient numbers in various geographic regions
Just how many aHUS patients are there? (March 2017)
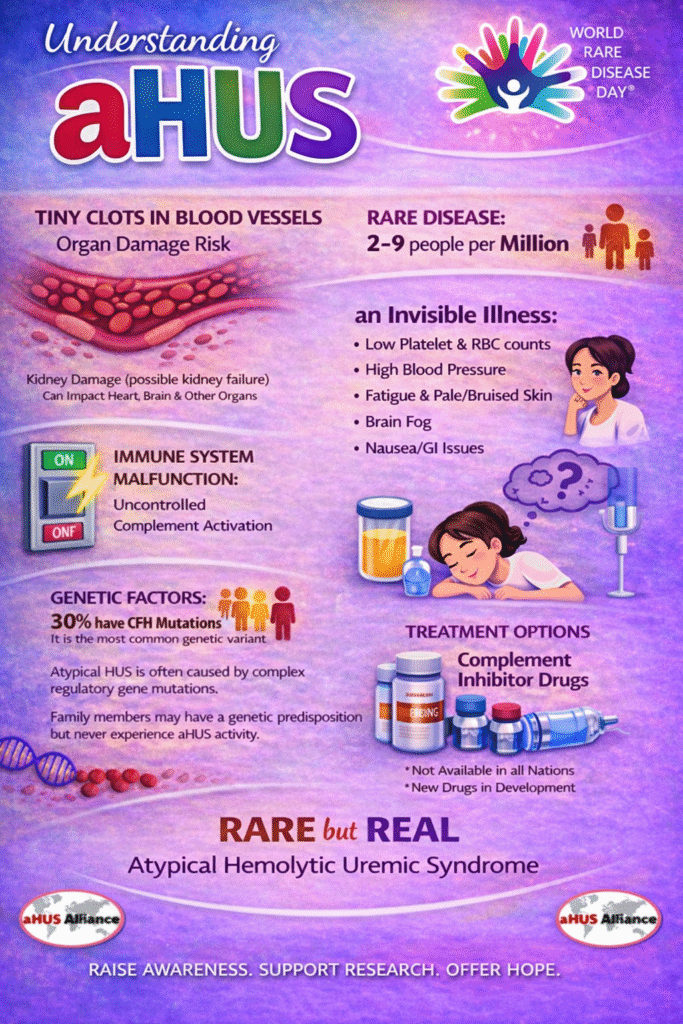
Rare But Real infographic – What is aHUS?